When I worked on community mobilization in a USAID-funded project in western Serbia two decades ago, developing ‘community social service projects’ was a challenge because of the perceptual divide between villagers and the experts in social services, education and health care. The villagers thought they didn’t know enough to develop such ideas, while the experts seemed to lack good connections to the villages to know what was most needed.
One of the projects has always remained with me. It was called “Save the Life” and it had very personal origins for one of our community facilitators, who had undergone surgery in Belgrade because the colposcope in her local community was defective. She was a brilliant facilitator and a lovely human being, who deeply understood the dynamics of her community.
So she brought both cultural and medical awareness to her design of the project. The first step was to find the cases of cervical cancer – challenging, because people in Serbia (at least then) didn’t speak of cancer. We could bring in doctors from the big city to do weekend clinics, but how to get the women to come? So she spoke with Orthodox clergy and persuaded them to speak about this at church – to urge men to persuade their wives, daughters and mothers to attend the clinics to save their lives. It was a brilliantly successful approach, and it saved many lives.
I remembered that facilitator’s wisdom – and how other Serbian women I met had developed specialized strategies to help treat ‘women’s’ ailments, circumventing cultural prohibitions on speaking of cancer – when I was reading about the success of the vaccine against human papillomavirus (HPV).
Cervical cancer, one of the few human cancers known to be directly caused by a viral infection, is the fourth most common cancer among women. Worldwide, a woman dies from the disease every 30 seconds, and 90% of the world’s estimated 300,000 cervical cancer deaths a year occur in women who live in low and middle-income countries where access to public health services is limited and screening and treatment have not been widely implemented.
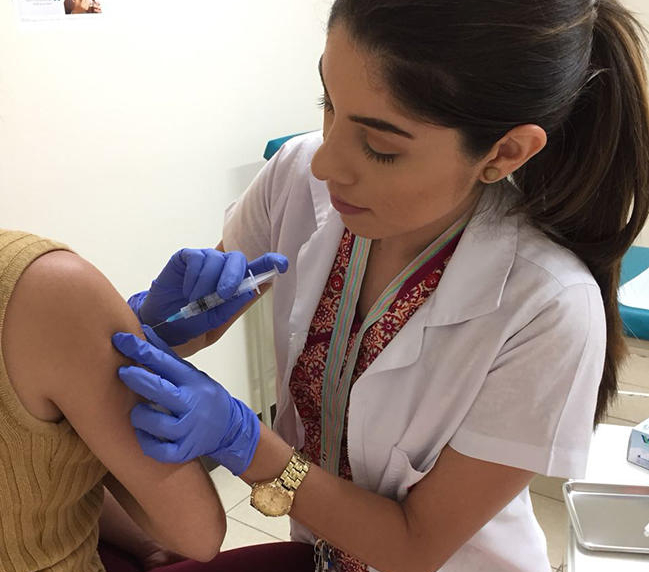
Yet now, HPV vaccination and screening for, and treating precancerous lesions, can prevent most cases, says the World Health Organization. “With a comprehensive approach to prevent, screen and treat, cervical cancer can be eliminated as a public health problem within a generation.”
In 2018, WHO announced a global call for action to eliminate cervical cancer, and in 2020, the World Health Assembly adopted the Global Strategy for cervical cancer elimination to guide its elimination as a public health problem.
This bold goal became possible because Australian immunologist Ian Frazer developed vaccines to fight cervical cancer – the first cancer vaccine – after decades of research by Frazer and his research partner Dr. Jian Zhou. In 1990, they began synthesizing particles that mimicked HPV, from which the vaccine would later be made.
Prof. Frazer was keen to see the vaccine become readily available to women worldwide. “The vaccine is designed for the developing world,” he said in 2006. “It will be sold first in the developed world, and of course there is a significant benefit for women in countries with effective Pap smear programs, as abnormal smears will be much less likely after vaccination, but the real need is for the developing world and to have this vaccine used routinely in young women to prevent cervical cancer in countries where there are no Pap smear programs to reduce the risk.”
Since 2018, Australia’s school based National Immunization Program has used Gardasil 9, which protects against nine types of human papillomavirus that cause around 90% of cervical cancers in women (and most other HPV-related cancers in women), 95% of all HPV-related cancers in men and 90% of genital warts across genders. It replaced Gardasil, which protected against four HPV types and was used between 2007 and 2017.
Australia, which has set a goal of eliminating cervical cancer by 2035, has taken steps to deal with one of the barriers – reluctance to get tested – by introducing self-collection cervical screening tests alongside the new HPV screening tests that replaced the pap smear. In November 2022, the University of Queensland renamed its UQ Diamantina Institute as the Frazer Institute, to honour Frazer’s co-invention of a world-first HPV vaccine which has already protected millions of women from cervical cancer – and will protect millions more in coming years.

Emeritus Professor Ian Frazer, University of Queensland
In 2020, a Swedish study of nearly 1.7 million women confirmed that widespread use of the HPV vaccine dramatically reduced the number of women who would develop cervical cancer. In girls vaccinated before age 17, there was a nearly 90% reduction in cervical cancer incidence during the 11-year study period (2006 through 2017) compared with women who had not been vaccinated. “This is a vaccine against cancer, which can save lives,” said the study’s leader, Jiayao Lei, Ph.D., of the Karolinska Institute in Stockholm.
In 2021, a UK study which looked at all cervical cancers diagnosed in England in women aged 20 to 64 between January 2006 and June 2019 showed that the vaccine reduced incidence by 34% in those who received it aged 16 to 18, 62% if aged 14 to 16 and 90% in those vaccinated aged 12 to 13. The UK implemented a HPV vaccine program for teenage girls in 2008.
“Primary prevention of cervical cancer is best achieved by high levels of HPV immunization among girls aged 9–14,” WHO said, urging all countries to introduce HPV vaccines to protect more girls and women from cervical cancer and all its consequences over the course of their lifetimes. Vaccination of boys, where feasible, also increases protection of girls through herd immunity and protects boys against other HPV-related cancers, it added.
In 2022, after Serbia and three other middle income countries launched nationwide vaccination of adolescents against HPV, girls in more than half of the middle income countries in WHO’s European region now have access to the life-saving vaccine.
Sources:
Equitable access to cervical cancer prevention in the WHO European Region increases as 4 more countries introduce HPV vaccination. WHO, Nov. 16, 2022
Noman is an island – race to end HPV.
Eliminating cervical cancer. WHO
Follow Australia’s lead: WHO calls for help in global cervical cancer fight. The Age, Nov. 19, 2021
Government commits another $5.8m to eliminate cervical cancer by 2035. The Sydney Morning Herald, Nov. 17, 2021
